New AI Model REDMOD Detects Pancreatic Cancer Earlier Than Ever
Pancreatic cancer has long been one of medicine’s most feared diagnoses — not just because of its aggression, but because of how silently it grows. Pancreatic ductal adenocarcinoma (PDAC) has a poor rate of survival. It’s usually diagnosed late, in the absence of symptoms and visible tissue changes in the early stages, and it rapidly progresses.
The numbers are sobering. Around 67,530 Americans are expected to be diagnosed with pancreatic cancer in 2026. It carries a very poor prognosis — around 13% survival at five years — largely because it is so often diagnosed at a late stage. And pancreatic cancer is on course to become the second-leading cause of cancer-related death in the US by 2030, in part because 85% of cases aren’t diagnosed until the disease has already spread.
Enter REDMOD: The AI That Sees What Humans Can’t
Researchers at the Mayo Clinic and the University of Texas MD Anderson Cancer Center have developed a powerful new AI framework to tackle this problem head-on. The system is called the Radiomics-based Early Detection Model (REDMOD), designed specifically to pick up the subtle tissue texture patterns — known as radiomics — of very early pancreatic cancer, which standard computed tomography (CT) scans simply cannot detect.
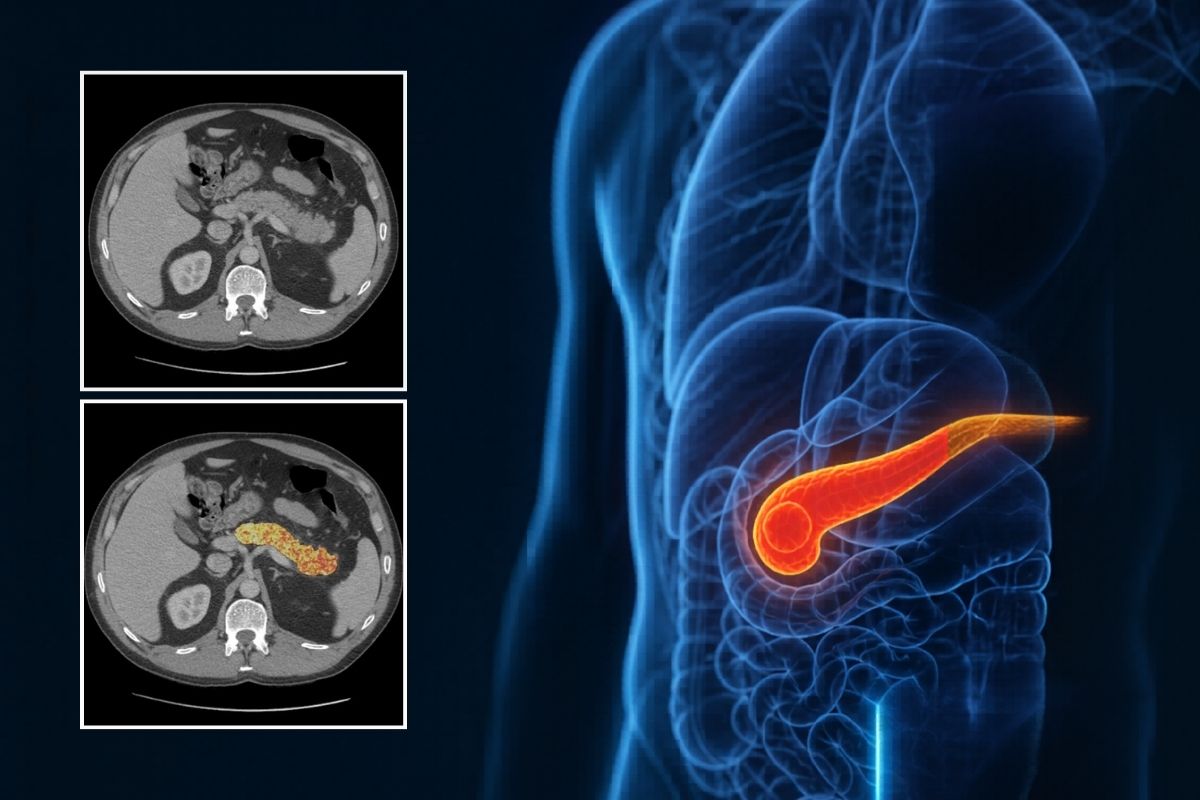
REDMOD measures hundreds of quantitative imaging features that describe tissue texture and structure, capturing faint biological changes as cancer begins to develop. The model is designed to analyze CT scans already obtained for other reasons — meaning it can work with existing imaging data without requiring any additional procedures or costs for patients.
Published in the journal Gut in April 2026, the findings imply artificial intelligence may be able to detect pancreatic cancer on normal belly CT images long before the tumors are detectable to human radiologists.
The Numbers That Are Turning Heads
The study’s findings are striking. Researchers used the AI model to analyze nearly 2,000 CT scans, including scans from patients later diagnosed with pancreatic cancer — all originally interpreted as normal. The system identified 73% of those pre-diagnostic cancers at a median of about 16 months before diagnosis — nearly double the detection rate of specialists reviewing the same scans without AI assistance.
Even more amazing is the fact that the edge was even bigger in the past. The AI found almost three times as many early cancers that would not have been found otherwise in scans done more than two years before the diagnosis.
To put it simply, REDMOD found pancreatic cancer a median of 475 days before a histopathologic diagnosis. This shows a clinically significant window for earlier action and possible survival gain.
What Makes REDMOD Different?
Unlike traditional radiology, which relies on a trained human eye spotting visible lesions, REDMOD works at a microscopic textural level. The framework includes automated pancreatic segmentation — clear delineation of the borders of the pancreas from surrounding tissue and organs — removing the need for this to be done manually and reducing the risk of variable accuracy.
As lead researcher, Dr. Ajit Goenka of the Mayo Clinic explained: “The greatest barrier to saving lives from pancreatic cancer has been our inability to see the disease when it is still curable. This AI can now identify the signature of cancer from a normal-appearing pancreas, and it can do so reliably over time and across diverse clinical settings.”
Who Could Benefit Most?
“For high-risk populations such as new-onset diabetes or chronic pancreatitis, this technology adds a new layer of surveillance. This method might help move diagnosis from the traditional late-stage, frequently fatal finding to far earlier identification at stage 0, when therapy is more likely to work, the researchers believe.
What Comes Next?
The researchers aim to test the AI on bigger and more varied groups of patients and determine how readily doctors can integrate it into what they’re already doing. As with every screening test, there is a potential for false positives that may lead to undue concern or further treatments. It is not meant to be the only basis of therapy, but to help guide the clinical monitoring.
Still, the medical community’s optimism is hard to contain. As the journal Gut study authors note: “Early detection of pancreatic ductal adenocarcinoma is the most powerful approach to improve survival.” REDMOD may have just made that a reality.

